A day at the COVID19 front line at the QEH King's Lynn
Our reporters spent the day on the Covid frontline at the Queen Elizabeth Hospital seeing its mantra of “The Safest Possible Care” in action.
Despite being exhausted both mentally and physically, the team spirit and morale of the staff is surprisingly unshakeable, even when faced with unprecedented and devastating circumstances.
Heartbreaking scenes on the wards, with patients struggling to breathe on CPAP machines, and taking more than an hour to eat a small pot of ice cream as their oxygen levels plummeted highlighted the devastating effect of the virus.
Given unprecedented access, we spoke to staff from every department, ranging from ICU consultants to the domestic team and came back with a sombre message.
“This is affecting young people, people in their 30s and 40s, people with no health problems; we have even watched our own colleagues deteriorate in front of us.
“Please follow the rules, no one is immune and this virus is an enigma - there’s no telling who will be affected in many cases.”
Hospital trust chief executive Caroline Shaw said: “We feel for the families too, every loss they suffer is heartbreaking. We share in their grief.
“With this new strain we have seen the staff infection rate go up from five per cent to 12 per cent and this is representative of the national figures as the new strain is 70 per cent more transmissible.”
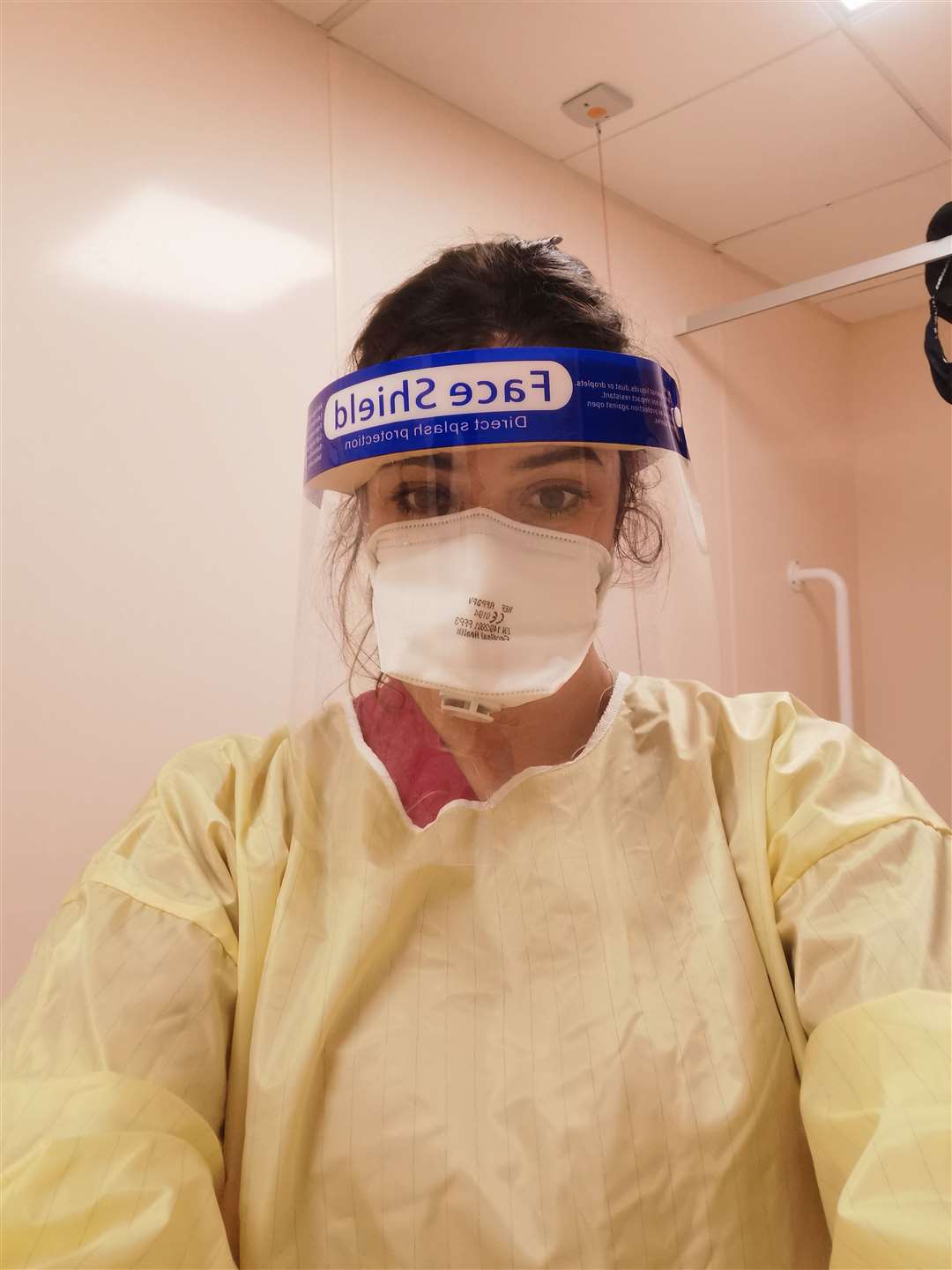
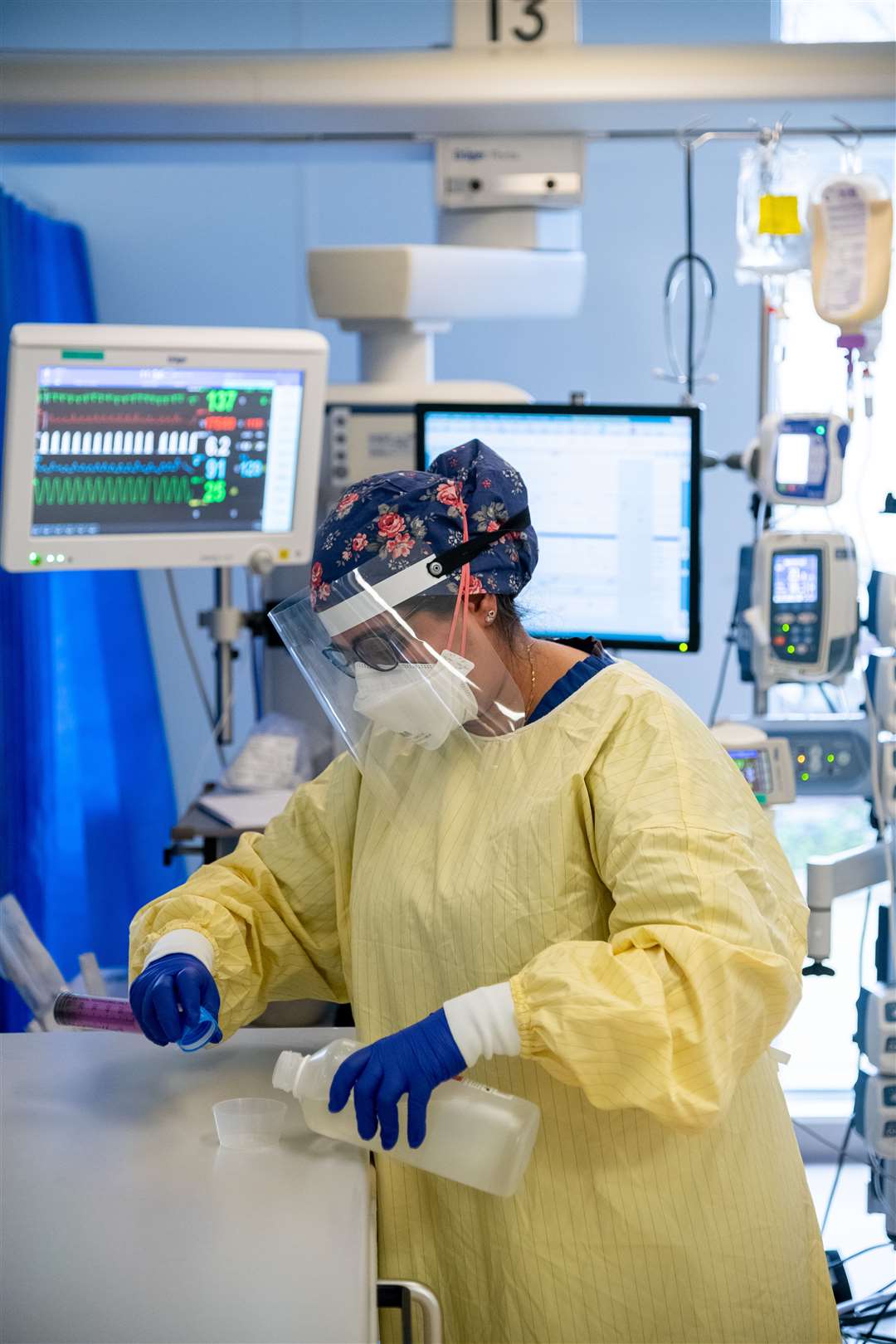
The PPE regulations are strict and escalate according to ‘zone’.
A red zone, which houses Covid-positive patients, has higher levels of PPE. The PPE is restrictive, giving a feeling that you can’t breathe properly, and some staff are wearing it for hours on end as they care for critical patients.
The ICU is at full capacity, and the porters say they “have never taken so many of our patients to the mortuary”.
The number of patients who have died at the QEH since the pandemic began last year this week climbed over 300 with seven more deaths confirmed on Wednesday. The total figure yesterday stood at 307.
It has become the ‘new normal’ for the nurses on the Tilney Covid-19 ward to see patients deteriorate rapidly on a daily basis with the virus, despite being otherwise healthy.
However, since the new strain has been infecting more people, the nurses warn of a frightening reality they are facing every day- patients are getting younger and younger.
“The youngest we’ve had was a 16 years old,” said Mia Elston, the ward manager.
“We are now seeing families, husbands and wives people in their 30s,40s and 50s. It’s heartbreaking.”
Karon Strong, Matron of Tilney ward explained the horror her team have dealt with: “On Monday morning a member of my team had to remove three wedding rings after death.
“That’s not a normal Monday. We keep on fighting and we have to be strong, but it’s so hard not to hug people or give them human contact when they are suffering.”
Mia and Karon took me into an isolated room to meet Covid patients Michael Hobbs, 49, a bus driver from Fakenham and Geoff Coone, 51, a council worker from Lynn.
These patients bravely shared their ordeal, despite being hooked up to CPAP (Continuous positive airway pressure) machines.
Michael, who was coughing and struggling to breathe, said he started to “feel bad” the week before and took a test.
Mere days later he is on Tilney ward being cared for by Mia and her team.
“I’m finding it very hard to breathe,” said Michael, who has a family at home. I hadn’t seen a doctor for years before this. I haven’t been unwell.”
Geoff, who was about to eat his lunch was switched from CPAP to oxygen in order to eat.
His oxygen drop severely within seconds of his CPAP mask being removed, from 90 per cent to below 60 cent.
“Forty per cent is not viable for life,” Karen aid, “It can take over an hour to eat a small tub of ice cream as we have to keep switching between masks. It’s so hard for them.”
Geoff wanted to tell his story: “I was still going into work, and a colleague’s partner had Covid, he didn’t bother to disclose that to any of us until it was too late.
“It makes me so upset. People just walk around like it doesn’t matter people need to stick to the rules and stay at home.”
This was a strong and poignant message, as we watched Geoff suffering and barely able to eat or breathe.
Emma, a nurse on the ward emotionally appealed to the public: “Please stay at home. I keep it together when I am here, but I drop my children off at school and see mums in the playground ignoring the rules and I think to myself ‘There are women your age in here that we are looking after’.”
The team praised the psychology department for their support, as many staff are offered trauma counselling for what they are dealing with on the wards.
Karen said: “They have been brilliant. Yes, we are all physically drained and working flat out but the mental impact takes it’s toll.”
Emma said, “We are strong at work and we carry on and we try our best when we go home not to let it affect us, but, of course, it does.”
Dr April Brown, chief nurse said: “I couldn’t be more proud of our team and how they are doing, their work is incredible and so valuable.”
It was a harrowing sight to step on to the red ICU ward with consultant Dr Peter Young, who has worked at the QEH for years.
Rows of ventilated patients lined the ward, most in their 50’s and 60’s, with some needing intrusive surgeries like tracheotomies to keep them alive.
One woman who had been on ventilation ‘for weeks’.
Some patients were ‘proned’, that is laid carefully on their front to maximise thoracic ventilation, which according to Dr April Brown, takes about eight people to execute.
On ICU survival rates, Peter said: “Last time it was about 60 per cent survival, but this time we have seen it go up.”
We saw one woman, who was concious who looked to be in her 30s.
Dr Raghu Govindan, the deputy medical director said: “The youngest we’ve had on ICU has been 36, however I am keen to point out that ICU admission largely depends on several factors.”
It is well known that conditions such as diabetes, hypertension and obesity contribute to having a higher risk of Covid complications. Dr Govindan said: “These are still the main things that we are seeing, yes this disease is somewhat of an enigma, but with these conditions there is a level of predictability in some cases, which is sad but happens to be the reality.”
Dr Young said: “We have had colleagues on ICU with us; one week they could be sitting (socially distanced, of course) in a meeting with us, and the next week we could be treating them.
“We have a lot to learn about this virus, but as we keep fighting it we are learning more and more.”
Dr Govindan said: “Before we ventilated everybody, but now our care is much more patient-based we decide with multi-disciplinary meetings about the use of ventilation and oxygen.”
Dr Young has implemented the launch of several new technological systems to help ICU staff conduct their work effectively and safely, one of which being the ‘Call for help’ App.
Each patient has a phone next to their bed and the doctors and nursing staff can be called on swiftly if their is any patient escalation.
This innovation can help many lives.
Our reporter met with the domestic team headed by Donna Mason and the portering department to hear how they are working just as hard as medical staff in the pandemic fight.
People often think of the nurses and doctors who are treating patients on the front line, but a large portion of staff, which includes cleaners and porters, are just as vital in their contribution to the safety of the patients and staff in the hospital.
Donna, echoing sentiments of pride felt throughout the QEH, said of her hard-working team: “Without them, we wouldn’t be able to do this.
“They ensure the hospital is safe at all times and work tirelessly and constantly to control the spread of infection, I am so, so proud of them, we won’t let this virus break us.”
Kelly Wells, is part of the cleaning team. She said: “We came into this job thinking maybe it was just cleaning, but it’s so much more than that, we have seen things that we never thought we would see, and we’ve kept going there’s such a strong team spirit we support each other.
“You just have to put your big girl pants on and do the job; yes, it’s scary but we have to get on with it.”
“I feel safer here than going into the supermarket, because I have confidence in how clean it is.”
Cheryl Brit, who was a hairdresser by trade, joined the ranks of the domestic team during the first wave: “Working here makes you step up with cleaning when you go home because it’s so important.
“We don’t know what to expect when we come to work, and we aren’t trained like nurses and doctors to deal with seeing all of this, but somehow we do it.”
Trudi Freear and Bradley Littlewood, who are dressed in black, are special infection control cleaners.
Bradley said: “It’s so much more than just cleaning, it’s about the safety and our team is fantastic we brighten each other’s day.”
Trudi said: “Doing this job opens your eyes to the reality of the virus.”
Porters Richard Geoffrey Cook,36, Zul Mangou,43 and Geoff Floyd,67 are responsible for transporting patients who have died to the mortuary, moving patients in beds and trolleys and handle the delivery of oxygen have had one of their team in ITU.
“It’s frightening,” said Geoff. We have 10 times the amount of work we used to have because now it’s not only Covid patients.”
Richard and Zhu spoke of the increase in visits to the mortuary: “We’ve seen so many, we try our best to be cheerful for each other and keep going but it doesn’t stop us being scared.”
The staff at QEH could not praise the clinical psychology team enough for supporting them through the pandemic.
We met with Dr Jo Burrell the Clinical Psychology Lead and Dr Steve Green a Clinical Psychologist to understand the importance of mental health wellbeing for all QEH staff as well as the general public.
Steve said: “It’s normal to have a trauma reaction to this, it’s what makes us all human. The staff have been kept in a Covid bubble and of course they have invasive traumatic images from what they have seen.”
Jo said: “We have been training mental health first aiders such as Katie Taylor from the communications team, to make sure staff are ok.
“We are keen to avoid labelling people with PTSD too soon although some are showing signs of it.
“We are offering CBT sessions and even a drop in service for those who want a shoulder to cry on.”
Steve said: “During the pandemic we have seen a sharp rise in mental health issues and we want to remove the stigma around it.”
The team had advice for the general public to handle pandemic anxiety in these nervy times.
Jo advised: “Connect with what you love whether it’s reading a hobby or music, take time away from horror stories, everyone knows the facts and if you are following the guidelines you have to focus what is within your control.
“This pandemic has taught people that looking after the mind is as important as looking after the body, and that’s why we’ve extended support for the staff who need us so they can carry on facing the day.”